The AHSN Network is celebrating the five-year anniversary of magnesium sulphate being introduced to reduce the incidence of brain injury and cerebral palsy in preterm infants. Thanks to the continued commitment of every perinatal team in England, more than 16,000 preterm babies and their families have benefitted.
Patient Safety Collaboratives (PSCs), commissioned by NHS England Patient Safety Team, have been working to increase adoption of the maternity and neonatal optimisation bundle for preterm infants since 2018. Magnesium sulphate is one of seven elements in the PReCePT bundle.
Initially, this work was known as PReCePT (Prevention of Cerebral Palsy in Preterm Labour), a two-year nationwide programme implemented between 2018 and 2020. Since PReCePT ended, the PSCs have continued to work with maternity units to support the adoption of all seven interventions. Magnesium sulphate use has continued to be used by 100% of maternity units.
A baby suffering avoidable harm, such as cerebral palsy, is a tragedy for everyone involved and the costs to the affected individual, their family and carers are immeasurable. The average medical litigation cost to NHS Resolution for each baby affected by cerebral palsy is £10,800,000, with an annual cost to the NHS of £1.8 billion.
Giving magnesium sulphate preterm labour has delivered the following outcomes:
- For every 37 women receiving magnesium sulphate, one fewer baby will be affected by cerebral palsy.
- 13,584 eligible women have received magnesium sulphate, protecting more than 16,000 babies (including multiple births), resulting in an estimated 367 fewer cases of cerebral palsy.
- Since 2018, this work has resulted in financial cost avoidance of up to £367 million (based on cost avoidance of between £0.8 to £1 million lifetime costs per affected baby with cerebral palsy). The magnesium sulphate injection itself costs just £1.

Magnesium sulphate uptake has increased over time, rising to a national average between 2021 and 2022 of 88.5% of eligible women being treated, with a range between PSCs of 86.8% to 92.1%. This means that every single PSC in England has reached and sustained the original 85% ambition. Seven out of fifteen PSCs have impressively achieved more than 90% magnesium sulphate take-up rate for eligible women.
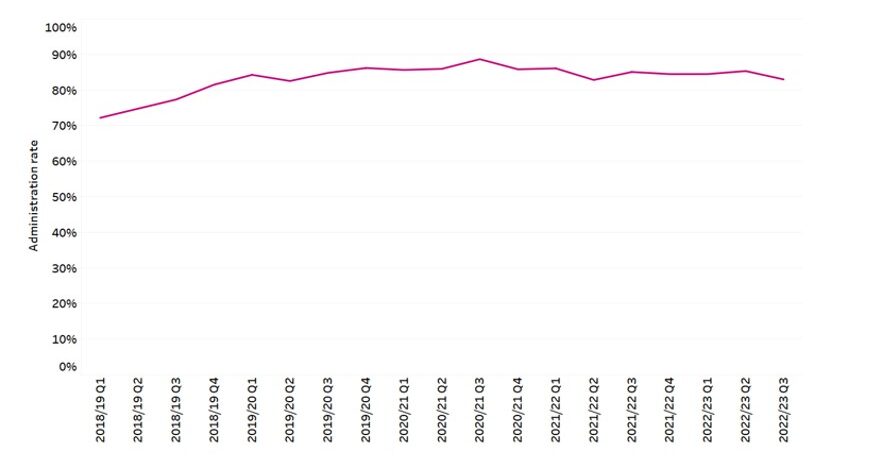
Magnesium sulphate administration
Dr Cheryl Crocker, AHSN Network Patient Safety Director, said:
“We are so proud of the work we do to prevent harm to mothers and their babies, but the real hard work is done by the front-line maternity and neonatal teams who support pregnant women. We are indebted to them for working with us, particularly during these high-pressure times and yet they still strive to provide a safe service.”
Professor Karen Luyt, National Clinical Lead for PReCePT, commented:
“Five years ago, we all shared the vision and goal to give every preterm baby the best start in life through magnesium sulphate neuroprotection. Now, in 2023, we can look back and say we have achieved and sustained our goal despite COVID-19 and its aftermath, thanks to the magnificent, sustained efforts of midwives and obstetric colleagues in every corner of our nation. You continue to make a real difference to the lives of babies and their families.”
- Find out more about the maternity and neonatal safety programme.
- Read about the PReCePT evaluation.

There is a wealth of HealthTech innovators poised to help solve some of the NHS’ greatest challenges, yet getting a product or new technology adopted at scale in the NHS is far from straightforward. In a recent ABHI member’s survey*, procurement was cited as one of the biggest barriers that innovators face, particularly those from [...]

Tellmi is a social enterprise innovation which aims to address the growing demand for mental health services and tackle health inequalities for young people. It is a digital peer support app available launched in 2017 by psychologist Suzi Godson PhD and engineer Kerstyn Comley PhD. Kersytn explains how Tellmi works. Tell us about the innovation. [...]

The NHS is facing record demand for services. According to The Health Foundation, the NHS waiting list for elective treatment in England has almost tripled in size over the last decade to 7.7 million. And latest figures show there were a record 2.35 million attendances at A&E across England in March this year. We know [...]







