Sickle cell patients have helped identify key priorities to improve access to treatment across England.
Published in a new report entitled ‘Appropriateness in access to automated red cell exchange: the patient perspective’, the five priority areas within the sickle cell treatment pathway that require attention and improvement are:
- Informed decision-making and talking to clinicians;
- Out of hours care for sickle cell
- Travel and transport arrangements
- Barriers in attending treatment: pain, fatigue and waiting times
- Pain relief: waiting times, under prescribing and overdose
The findings in the report stem from data obtained from a national survey and insights gleaned from a webinar attended by clinicians and patients living with sickle cell disease.
This research was a collaboration between NHS England’s Patient and Public Involvement and Engagement Team in the Innovation, Research and Life Sciences Group, Haemoglobinopathy Coordination Centres, the Sickle Cell Society, and Health Innovation Yorkshire & Humber.
In the UK, approximately 15,000 individuals live with sickle cell disease, a debilitating condition that significantly impacts people’s lives. People living with this disorder can experience episodes of severe pains and are at greater risk of complications such as stroke, acute chest syndrome, blindness, or bone damage.
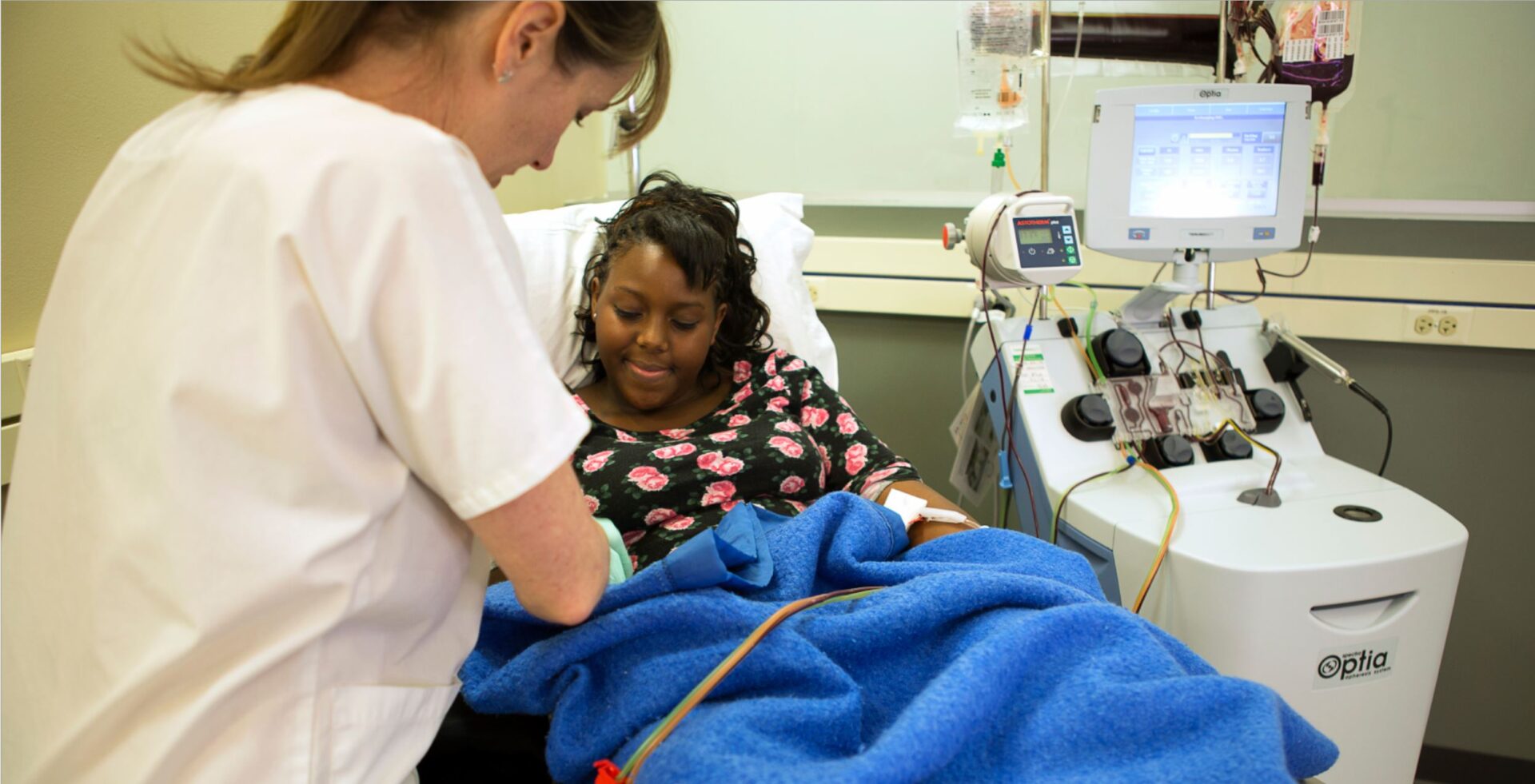
As part of NHS England’s MedTech Funding Mandate policy, the Health Innovation Network was tasked with increasing access to Spectra Optia® Apheresis System device, one of the technologies supported through the programme, addressing longstanding inequalities reported by patients in accessing the right care.
A number of initiatives have already been implemented. These include work with Terumo, the manufacturer of the Spectra Optia® Apheresis System device, and the Sickle Cell Society to produce an avatar in English and French to help patients understand their treatment options, and how automated red blood cell exchange is not just for emergencies, but can be accessed routinely every few weeks by eligible patients.
Harriet Smith, National Programme Lead for Spectra Optia, at Health Innovation Yorkshire & Humber, said: “It’s imperative that we collaborate to ensure universally excellent care and treatment, regardless of one’s location or identity. The insights gained from the national survey provide a roadmap for positive change.”
John James OBE, CEO of the Sickle Cell Society, added: “In the journey to transform sickle cell care, patient-centred solutions are paramount. By addressing the key challenges revealed in our national survey we pave the way for a more inclusive and effective healthcare system.”
Zoe Hamilton, National Programme of Care Manager, Blood & Infection, Specialised Commissioning NHS England, added: “Incorporating the perspectives and experiences of patients in the design of health and care services is essential. Patient involvement ensures that services are not only medically effective but also genuinely responsive to the diverse needs, preferences, and challenges faced by individuals, fostering a more compassionate, person-centred approach to healthcare.”

There is a wealth of HealthTech innovators poised to help solve some of the NHS’ greatest challenges, yet getting a product or new technology adopted at scale in the NHS is far from straightforward. In a recent ABHI member’s survey*, procurement was cited as one of the biggest barriers that innovators face, particularly those from [...]

Tellmi is a social enterprise innovation which aims to address the growing demand for mental health services and tackle health inequalities for young people. It is a digital peer support app available launched in 2017 by psychologist Suzi Godson PhD and engineer Kerstyn Comley PhD. Kersytn explains how Tellmi works. Tell us about the innovation. [...]

The NHS is facing record demand for services. According to The Health Foundation, the NHS waiting list for elective treatment in England has almost tripled in size over the last decade to 7.7 million. And latest figures show there were a record 2.35 million attendances at A&E across England in March this year. We know [...]